 The heart will beat independently of any nervous or hormonal influences.
The heart will beat independently of any nervous or hormonal influences.
The spontaneous rhythm of the heart is called intrinsic automaticity and can be altered by nervous impulses or by circulatory substances, like adrenaline.
The muscle fibres of the heart are excitable cells like other muscle or nerve cells and each have a unique property.
The cells in the heart will spontaneously contract at a regular rate because the electrical properties of the cell membrane spontaneously alter with time and regularly “depolarise”. This depolarisation means reversal of the electrical gradient across the cell membrane. That reversal in electrical gradient causes muscle contraction or conveyance of a nervous impulse.
Muscle fibres from different parts of the heart have different rates of spontaneous depolarisation; the cells from the ventricle are the slowest, and those from the atria are faster.
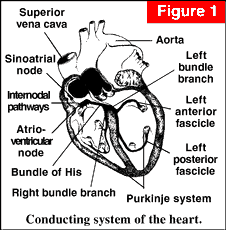
Electrical activity then passes through the AtrioVentricular node (AV node) and through into the ventricles via the Purkinje fibres in the Bundle of His to produce a ventricular contraction.
If there is any disease of the conducting system of the heart, then this process may be interfered with and the heart rate altered. If, for example, there is disease of the AV node, then there is an electrical block between the atria and the ventricles. The ventricles will beat with their own inherent rhythm, which is much slower, usually 30-50 beats per minute.
Anaesthetic drugs, like halothane, may depress the rate of depolarisation of the SinoAtrial node, and the AtrioVentricular node may then become the pacemaker of the heart. When this occurs it is frequently termed nodal or junctional rhythm.
The automatic rhythm of the heart can be altered by the autonomic nervous system.
The sympathetic nervous system connection to the heart leaves the spinal cord at the first four thoracic vertebra, and supplies most of the muscle of the heart. (see ANS diagram)
Stimulation via the cardiac beta-1 receptors causes the heart rate to increase and beat more forcefully.
The vagus nerve also supplies the atria, and stimulation causes the heart rate to decrease (bradycardia).
Surgical procedures can cause vagal stimulation and produce severe bradycardia. Examples include pulling on the mesentery of the bowel, anal dilatation or pulling on the external muscles of the eye.
Under normal conditions the vagus nerve has the most influence on the heart. This is especially noticeable in athletes who have slow heart rates.
There are nervous reflexes that effect heart rate. The afferent’s are nerves in the wall of the atria or aorta that respond to stretch. The aorta contains high pressure receptors. When the blood pressure is high these cause reflex slowing of the heart to reduce the cardiac output and the blood pressure. Similarly, when the blood pressure is low, the heart rate increases, as in shock.
Similar pressure receptors are found in the atria.
When the atria distend, as in heart failure or over transfusion, there is a reflex increase in the heart rate to pump the extra blood returning to the heart.
When there is a sudden reduction in the pressure in the atria the heart slows. This is called the Bainbridge Reflex and is the cause for the marked bradycardia sometimes seen during spinal anaesthesia.
Circulatory substances can also affect the heart rate:
Catecholamines, like adrenaline, are released during stress, and will cause an increase in heart rate.
Drugs are another common cause of change in the heart rate and most anaesthetic drugs will do that.
Halothane affects the SinoAtrial node and will also depress the force of contraction of the heart.
Isoflurane, by contrast has little direct affect on the heart, but causes peripheral vasodilation of the blood vessels. Peripheral vasodilation will then decrease the blood pressure, and hence produce a reflex tachycardia.
Ketamine causes stimulation of the sympathetic nervous system, and therefore produces a tachycardia.
Other circulating substances may also affect the heart rate, acting indirectly through the autonomic nervous system. For example increased blood concentrations of carbon dioxide will cause stimulation of the sympathetic nervous system and tachycardia, and is an important sign of respiratory failure.
